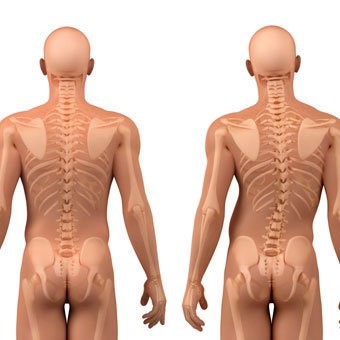
Scoliosis – Part 2
In my last blog, I explained the different types of scoliosis, how we screen for them and how we could see them presenting in ourselves, our friends and family. It is again, really important to note, that scoliosis is in most cases, not a life-threatening disease and we do not have to live in fear […]
Pre, During and Post Pregnancy Care
Pre, During and Post – Pregnancy Care is now available in Healthworks. During pregnancy, our centre of gravity shifts and this causes many to experience lower and upper back pain. This leads to stress and sometimes neck and headaches. With the help of adjustments and myotherapy, pain and discomfort can be relieved, making the experience […]
Cervicogenic Headache
Headache is an extremely common symptom and the most common of the nervous system disorders. Nearly 5 in every 10 individuals will be diagnosed with a headache. It affects the young and old, all races and genders, but mostly females. There are many types of headaches and amongst them, chiropractors have found that the trend […]
Physical Activity in Elderly
Aging is a multifactorial irreversible process associated with significant decline in muscle mass and neuromuscular functions. One of the most efficient methods to counteract age-related changes in muscle mass and function is physical activity. Lack of activity destroys the good condition of every human being, while movement and methodical physical exercise save it and preserve […]
Why Am I So Flexible?
Have you ever watched one of those videos where some people can extend their index finger till it reaches the back of the hand? How are some people way more flexible than others? Hypermobile joints which literally translate to joints with an excessive mobility, is often seen when the tissues holding a joint together – […]